Connect With Us
Blog

What is Achilles Tendinopathy?
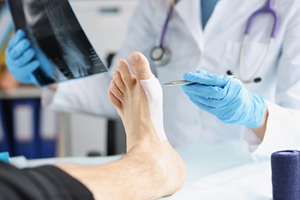
 Achilles tendinopathy is a condition characterized by pain, swelling, and stiffness in the Achilles tendon, which connects the calf muscles to the heel bone. This condition often results from overuse, particularly in athletes and individuals who engage in repetitive activities such as running or jumping. It can also arise from a sudden increase in physical activity, wearing poor footwear, or biomechanical issues like flat feet. The pain associated with Achilles tendinopathy usually starts as a mild ache above the heel or in the back of the leg, worsening with activity. The condition can range from mild inflammation to more severe degeneration of the tendon fibers. Diagnosis typically involves a physical examination and imaging tests, such as ultrasound or MRI scans to assess the extent of the damage. Treatment options include rest, targeted exercises, and nonsteroidal anti-inflammatory drugs. In severe cases, surgery may be required to repair the tendon. Preventative measures include proper warm-up routines, wearing appropriate footwear, and gradually increasing the intensity of physical activity. If you experience symptoms of Achilles tendinopathy, it is suggested that you schedule an appointment to see a podiatrist for an accurate diagnosis and effective treatment plan.
Achilles tendinopathy is a condition characterized by pain, swelling, and stiffness in the Achilles tendon, which connects the calf muscles to the heel bone. This condition often results from overuse, particularly in athletes and individuals who engage in repetitive activities such as running or jumping. It can also arise from a sudden increase in physical activity, wearing poor footwear, or biomechanical issues like flat feet. The pain associated with Achilles tendinopathy usually starts as a mild ache above the heel or in the back of the leg, worsening with activity. The condition can range from mild inflammation to more severe degeneration of the tendon fibers. Diagnosis typically involves a physical examination and imaging tests, such as ultrasound or MRI scans to assess the extent of the damage. Treatment options include rest, targeted exercises, and nonsteroidal anti-inflammatory drugs. In severe cases, surgery may be required to repair the tendon. Preventative measures include proper warm-up routines, wearing appropriate footwear, and gradually increasing the intensity of physical activity. If you experience symptoms of Achilles tendinopathy, it is suggested that you schedule an appointment to see a podiatrist for an accurate diagnosis and effective treatment plan.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of New England Foot and Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact one of our offices located in Chelmsford and Newburyport, MA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
The Causes, Types, and Treatments of Achilles Tendon Injuries
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.
Tips for Preventing Running Injuries

Whether you're a novice runner or a seasoned marathoner, injury prevention is a top priority. An important aspect of running injury prevention is having a structured plan and progressing slowly. Avoiding increasing your total mileage by more than 10 percent each week helps prevent overexertion and gives your muscles and ligaments adequate time to adapt. It's also essential to strike a balance between increasing distance and improving speed. Focusing on one aspect at a time can reduce the risk of overuse injuries. Proper hydration, replenishing your body with a combination of protein and carbohydrates within 30 minutes post-run, and practicing deep breathing exercises to stimulate a relaxation response can all aid in muscle repair and reduce soreness. Incorporating cross-training activities such as swimming or cycling into your routine provides a welcome break from the impact of running. Dynamic stretches before your run help prime your muscles for activity, while static stretches afterward improve flexibility and reduce the risk of injury. If you are experiencing pain from running it is suggested that you make an appointment with a podiatrist. This foot doctor can also perform gait analysis and assess biomechanical problems that may cause injuries.
All runners should take extra precaution when trying to avoid injury. If you have any concerns about your feet, contact one of our podiatrists of New England Foot and Ankle. Our doctors will treat your foot and ankle needs.
How to Prevent Running Injuries
There are a lot of mistakes a runner can make prior to a workout that can induce injury. A lot of athletes tend to overstretch before running, instead of saving those workouts for a post-run routine. Deep lunges and hand-to-toe hamstring pulls should be performed after a workout instead of during a warmup. Another common mistake is jumping into an intense routine before your body is physically prepared for it. You should try to ease your way into long-distance running instead of forcing yourself to rush into it.
More Tips for Preventing Injury
- Incorporate Strength Training into Workouts - This will help improve the body’s overall athleticism
- Improve and Maintain Your Flexibility – Stretching everyday will help improve overall performance
- “Warm Up” Before Running and “Cool Down” Afterward – A warm up of 5-10 minutes helps get rid of lactic acid in the muscles and prevents delayed muscle soreness
- Cross-Training is Crucial
- Wear Proper Running Shoes
- Have a Formal Gait Analysis – Poor biomechanics can easily cause injury
If you have any questions, please feel free to contact one of our offices located in Chelmsford and Newburyport, MA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Prevent Running Injuries
Overtraining and overusing the feet are the main causes of common running injuries. A number of these common injuries are caused by overrunning. Runner’s knee is a condition that is characterized by the back of the kneecap beginning to wear away and cause pain in the knee. This frequently occurs due to either a decrease in strength in the quadriceps muscles or ill-fitting shoes that are lacking in proper support for the inside of the forefoot. Strengthening exercises focusing on the quad muscle and sports orthotics are the usual treatments for those suffering from runner’s knee. Prevention of the condition lies in a focus on hip strengthening and quad-strengthening to keep the kneecap aligned. To help learn the best exercise to heal runner’s knee, one can also undergo physical therapy.
One common injury, called iliotibial band syndrome, is often caused by overtraining. This condition occurs when the iliotibial band gets irritated, creating pain and discomfort in the outside knee area. Plantar fasciitis, another common running injury, also occurs as a result of inflammation and irritation. Plantar fasciitis is an inflammation and irritation of the bone in the foot. A large amount of pain is often experienced due to plantar fasciitis. The condition can be caused by a high arch, improper footwear, tight muscles, or flat feet. It can best be avoided by stretching and wearing appropriate footwear that supports the foot.
Another common injury for runners is stress fractures. These injuries occur due to running style, overtraining, or a lack of calcium. Stress fractures most often occur in several locations in runners, including the inner bone of the leg, the thighbone, the bone at the base of the spine and the bones of the toes. Stress fractures are best prevented by wearing proper footwear and by running on flat and hard surfaces; this will absorb some of the shock created during running.
Aside from overtraining, other causes of common running injuries include ill-fitting footwear, a lack of flexibility and strength, and irregular biomechanics. The best way to avoid running injuries is to prevent them from even occurring. Both iliotibial band syndrome and stress fractures are preventable. The first step that should be taken to prevent running injuries is to only wear footwear that fits properly and that is appropriate for whatever activity you are doing. Running shoes are the only protective gear available to runners that can safeguard them from sustaining injuries. Choosing the right pair of shoes is therefore extremely important. While running shoes are an important factor, it is also important to consider other facets of your running routine such as training schedules, flexibility, and strengthening. These elements should be considered and altered according to your running needs to best maximize your run and minimize the possibility of injury. Careful stretching before and after a run should also be considered to help prevent running injuries. Stretching muscles enables greater flexibility and a lesser chance of sustaining injury.
Minor Foot Surgery
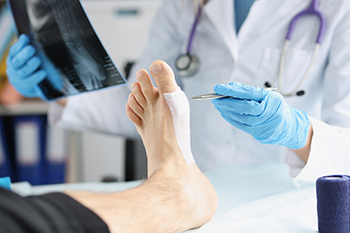 Minor foot surgery encompasses a range of procedures aimed at addressing common foot problems with minimal invasiveness. These surgeries are often performed to correct issues like ingrown toenails, bunions, hammertoes, and plantar warts. Ingrown toenail surgery involves removing part or all of the affected nails to relieve pain and prevent infection. Bunion surgery, or a bunionectomy, involves realigning the bone, ligaments, and tendons to correct the deformity. Hammertoe surgery aims to straighten the bent toe by removing a portion of the bone or releasing the tendon. Plantar wart removal can be performed using various methods, including excision, laser therapy, or cryotherapy. These procedures are typically done on an outpatient basis under local anesthesia, allowing for quick recovery and minimal downtime. If you have any sort of foot problem, it is suggested that you schedule an appointment with a podiatrist. After a thorough examination and imaging tests, the best treatment, which may include minor surgery, will be discussed.
Minor foot surgery encompasses a range of procedures aimed at addressing common foot problems with minimal invasiveness. These surgeries are often performed to correct issues like ingrown toenails, bunions, hammertoes, and plantar warts. Ingrown toenail surgery involves removing part or all of the affected nails to relieve pain and prevent infection. Bunion surgery, or a bunionectomy, involves realigning the bone, ligaments, and tendons to correct the deformity. Hammertoe surgery aims to straighten the bent toe by removing a portion of the bone or releasing the tendon. Plantar wart removal can be performed using various methods, including excision, laser therapy, or cryotherapy. These procedures are typically done on an outpatient basis under local anesthesia, allowing for quick recovery and minimal downtime. If you have any sort of foot problem, it is suggested that you schedule an appointment with a podiatrist. After a thorough examination and imaging tests, the best treatment, which may include minor surgery, will be discussed.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact one of our podiatrists of New England Foot and Ankle. Our doctors will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact one of our offices located in Chelmsford and Newburyport, MA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot Surgery
In most cases, foot surgery is often chosen as the last available option for conditions that have otherwise been unsuccessfully treated. Surgery may be necessary for several reasons, including the removal of foot deformities (e.g. bone spurs or bunions), arthritis problems, reconstruction due to injury, and congenital malformations (e.g. club foot or flat feet). Regardless of one’s age, foot surgery may be the only successful option for treatment for certain conditions.
The type of surgery one undergoes depends on the type of foot condition the patient has. For the removal of a bunion growth, a bunionectomy is necessary. If the bones in the feet need to be realigned or fused together, a surgical fusion of the foot is needed. For pain or nerve issues, a patient may require surgery in which the tissues surrounding the painful nerve are removed. Initially, less invasive treatments are generally attempted; surgery is often the last measure taken if other treatments are unsuccessful.
While in many cases surgery is often deemed as the final resort, choosing surgery comes with certain benefits. The associated pain experienced in relation to the particular condition is often relieved with surgery, allowing patients to quickly resume daily activities. The greatest benefit, however, is that surgery generally eliminates the problem immediately.
Podiatry history has shown that foot treatments continue to evolve over time. In the field of foot surgery, endoscopic surgery is just one of the many advanced forms of surgery. As technology vastly improves so too will the various techniques in foot surgery, which already require smaller and smaller incisions with the use of better and more efficient tools. Thanks to such innovations, surgery is no longer as invasive as it was in the past, allowing for faster and easier recoveries.
Strategies for Preventing Falls in the Workplace

In any workplace, the safety and well-being of employees are paramount, and preventing falls is a key aspect of maintaining a secure environment. Employers can implement various strategies to mitigate the risk of falls and minimize potential injuries. One effective method is to maintain a clean and organized workspace, free from clutter or obstacles that could cause tripping hazards. Ensuring proper lighting throughout the premises enhances visibility and reduces the likelihood of missteps. Additionally, installing handrails, guardrails, or non-slip surfaces in areas prone to falls, such as staircases or slippery floors, provides essential support and stability. Regular maintenance of equipment and infrastructure also plays a vital role in preventing accidents. Additionally, comprehensive employee training programs on fall prevention techniques and safety protocols empower workers to identify risks and take proactive measures. If you have a foot injury as a result of falling during your workday, it is suggested that you consult a podiatrist who can offer effective treatment options.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with one of our podiatrists from New England Foot and Ankle. Our doctors will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact one of our offices located in Chelmsford and Newburyport, MA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
Podiatrist’s Role in Diabetic Limb Salvage
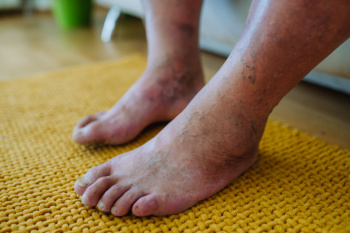
Podiatrists play an indispensable role in the realm of diabetic limb salvage by addressing not only the immediate wound but also the underlying biomechanical issues of the foot and ankle. These foot and ankle specialists view the diabetic wound in the context of the entire lower limb's structure and function, which involves meticulous local wound care. Debridement and the use of advanced topical therapies and bioengineered tissues, coupled with strategies to offload pressure from the wound site are included. Offloading techniques might include total contact casts, custom braces, and healing shoes with custom inserts designed to redistribute pressure and prevent further injury. When conservative measures fail, surgical intervention may be necessary. Procedures like Achilles tendon lengthening or tendon transfers are performed to rebalance the foot, addressing deformities and reducing abnormal pressures that contribute to ulcers. In more severe cases, reconstructive surgery may be needed to stabilize the foot and prevent ongoing damage. Postoperative care is critical to ensure long-term success, with custom footwear and regular biomechanical monitoring playing key roles in preventing recurrence. If you are experiencing diabetic foot ulcers, it is suggested that you schedule an appointment with a podiatrist for holistic care that heals the wounds and maintains the overall health and function of your feet.
Limb salvage can be an effective way in preventing the need for limb amputation. If you have diabetes, cancer, or any other condition that could lead to foot amputation if left unchecked, consult with one of our podiatrists from New England Foot and Ankle. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Limb Salvage?
Limb salvage is the attempt of saving a limb, such as the foot from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Diabetes is the number one cause of non-traumatic amputations in the United States. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
However, there are other causes as well, such as cancer and traumatic injury. Links between higher mortality rates and amputation have been found. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact one of our offices located in Chelmsford and Newburyport, MA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blog Archives
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- March 2016